Key Takeaways
- OCD rumination is a mental compulsion, not just overthinking.
- It feels like problem-solving, but it is actually part of the OCD cycle that keeps anxiety alive.
- The more you ruminate, the more uncertain you feel.
- Rumination is driven by a need for certainty and a desire to get rid of anxiety but it has the opposite effect.
- Recovery involves changing your response to thoughts, not eliminating them.
- Approaches like ERP and ACT help you tolerate uncertainty and step out of the rumination loop.
Disclaimer: This article is for educational purposes, not medical advice.
OCD Rumination Explained
Rumination is not just “thinking too much.” It is a mental process where you try to solve, analyze, or get certainty about something that feels unresolved.
In OCD, rumination becomes a mental compulsion. It is an attempt to reduce anxiety, doubt, or discomfort by thinking things through again and again. Unlike visible compulsions, such as checking or washing, this happens entirely in your head, which makes it harder to notice.
OCD rumination often feels productive at first. It can seem like you are being responsible, careful, or thoughtful. But in reality, you are stuck in a loop of obsessive thinking that does not lead to resolution.
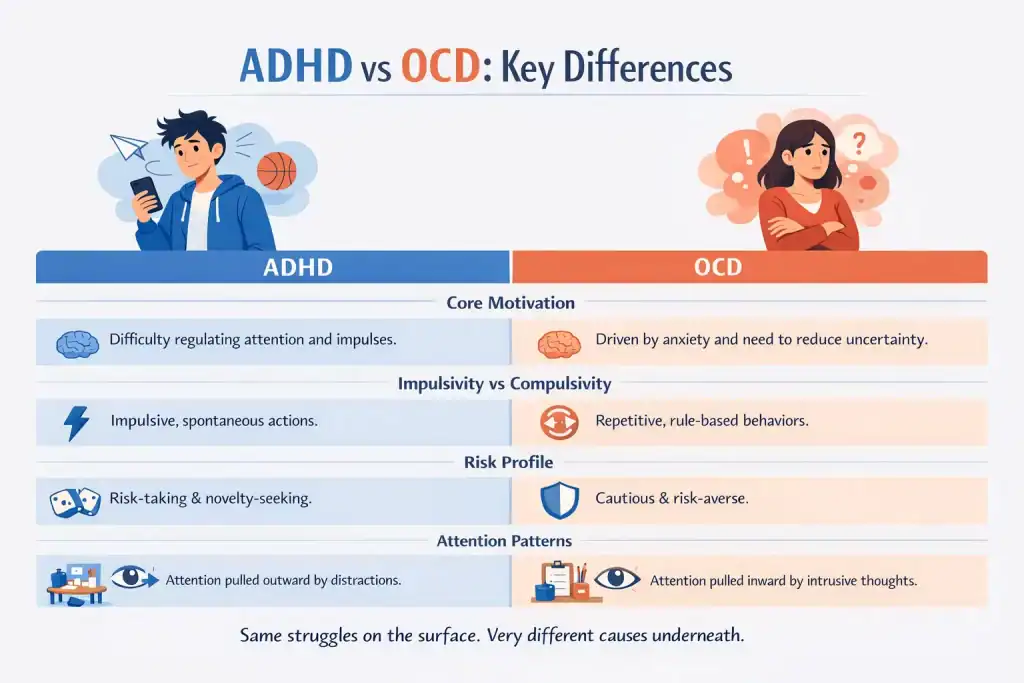
Rumination is also not unique to OCD. It appears in other conditions such as ADHD, anxiety, and depression. The key difference is that in OCD, it is driven by a need for certainty and relief from intrusive thoughts.
What Does OCD Rumination Feel Like?
If you have experienced OCD rumination, you will likely recognize the pattern immediately. It has a very specific “texture” in the mind.
Common traits include:
- Repetitive thoughts that feel impossible to settle.
- Distressing mental loops that create anxiety.
- A sense that the thinking is involuntary or hard to stop.
- An urge to resolve doubt or reach certainty.
- Going in circles without reaching a clear answer.
- Constant reviewing, analyzing, or replaying situations.
OCD rumination is not just thinking. It feels urgent. It feels like something needs to be figured out right now.
At the same time, there is a subtle awareness that the process is not helping. You may notice that no matter how much you think, the relief never lasts.
Is OCD Rumination the Same as Overthinking?
It is easy to confuse OCD rumination with overthinking, but they are not the same.
Overthinking can happen to anyone. It might involve worrying about decisions, replaying conversations, or imagining future scenarios. While uncomfortable, it is usually flexible and can stop when attention shifts.
OCD rumination is different.
It is compulsive
It is driven by anxiety and the need to eliminate uncertainty. The thinking feels necessary, almost like a responsibility. You may believe that if you do not fully think something through, something bad could happen or you could be making a serious mistake.
Another key difference is that OCD rumination tends to get stronger the more you engage with it. Instead of resolving the issue, it reinforces the cycle.
| OCD Rumination | Overthinking |
|---|---|
| Driven by anxiety and a need for certainty | Often driven by stress, curiosity, or decision-making |
| Focused on resolving doubt or preventing something bad | Focused on evaluating options or reflecting on situations |
| Repetitive and circular, going over the same thoughts again and again | Can move between different ideas or scenarios |
| Gets stronger the more you engage with it | Usually fades when attention shifts |
| Does not lead to resolution or relief long-term | Can sometimes lead to decisions or insights |
| Reinforces the OCD cycle | Does not typically create a self-perpetuating cycle |
Examples of Rumination in OCD
To better understand OCD rumination examples, it helps to look at how it shows up in different themes.
Relationship OCD
Daniel finds himself constantly analyzing his feelings toward his partner, which is a common OCD pattern known as Relationship OCD.
“Do I really love them?”
“What if I am lying to myself?”
“What if I am wasting their time?”
At first, it starts as a passing doubt. One evening, he notices he does not feel as connected as usual, or he catches himself comparing his relationship to someone else’s. The thought lingers longer than it should, and instead of letting it pass, his mind locks onto it.
He begins replaying conversations, searching for clues. Did I feel enough when they said “I love you”? Did I hesitate? Should I have felt something stronger? He studies their expressions, their tone, even small pauses, trying to extract certainty from each interaction.
The analysis spreads into everything. He compares his relationship to others, to movies, to past experiences. He tries to measure his feelings, hoping to reach a clear answer. But each time he gets close, a new doubt appears.
“What if I am just convincing myself?”
“What if I am missing something important?”
The more Daniel thinks, the less certain he feels. What once felt natural now feels forced and examined. Instead of being present in the relationship, he is stuck evaluating it, trapped in a loop that never quite resolves.
Harm OCD
María is washing dishes when an intrusive thought flashes through her mind. It is sudden and disturbing, completely out of line with who she believes herself to be. It involves harming a loved one, which is a common fear among people with Harm OCD.
For a moment, she freezes. Then the questioning begins.
Why would I think that? Does this say something about me? She tries to trace the thought back to its origin, searching for a reason that would make it feel less threatening. Maybe it was stress. Maybe she is just tired. But the explanations never feel convincing enough.
She starts reviewing her past. Has she ever acted aggressively? Has she ever come close to losing control? She replays memories, analyzing her intentions in each one, looking for proof that she is safe.
For brief moments, she feels relief. She tells herself she would never act on such a thought. But then doubt creeps back in.
“What if I am missing something?”
“What if this time is different?”
The urgency builds, pulling her back into the same mental loop. The more María tries to prove to herself that she is not dangerous, the more real the fear begins to feel. The process feels necessary, even responsible, but it never fully resolves the anxiety.
Real Event OCD
Lucas is traveling through China as part of a university program. One afternoon, he rents a bike with a couple of classmates and heads out for a ride near Guilin. As he cycles down a quiet road, he notices a young girl standing off to the side. He does not get a clear look at her, just a brief impression as he passes.
A thought appears. Is she okay? Does she need help?
He considers stopping, but his classmates are already ahead. If he stops, he might lose them. So he keeps going.
Later, back at the hotel, everyone is relaxed and talking. But Lucas is stuck on that moment. He begins replaying it in his head, trying to reconstruct what he saw. With each replay, the image changes slightly. Now she looks more distressed. Now she seems disheveled. Now it feels like something was clearly wrong.
The doubt grows heavier. What if she needed help and I ignored her? What if something bad happened because I didn’t act?
He spends hours going over the scene, analyzing every detail, trying to reach certainty. He tells himself that he will go back the next morning and find her. This is a classic example of Real Event OCD where the more he thinks about the issue, the more uncertain he becomes.
How to Stop OCD Rumination
It is not easy to stop ruminating, particularly if you are a person that has been diagnosed with OCD. The first step in stopping OCD rumination involves understanding something counterintuitive:
Rumination does not solve the problem. It only reinforces the OCD cycle
We ruminate because we believe it is a workable way to end the obsession and get rid of the anxiety. It makes sense to us that if we think hard enough, we’d be able to “solve” the issue. In reality, OCD obsessions cannot be resolved through logic or brute force, and rumination only help reinforce the vicious mental pattern known as the OCD cycle.
This cycle is simple:
- An obsession creates anxiety
- To placate the anxiety, we ruminate
- Rumination leads to short-term relief
- The obsession reappears because we did not solve the issue, which cannot be solved to begin with, and the cycle starts again
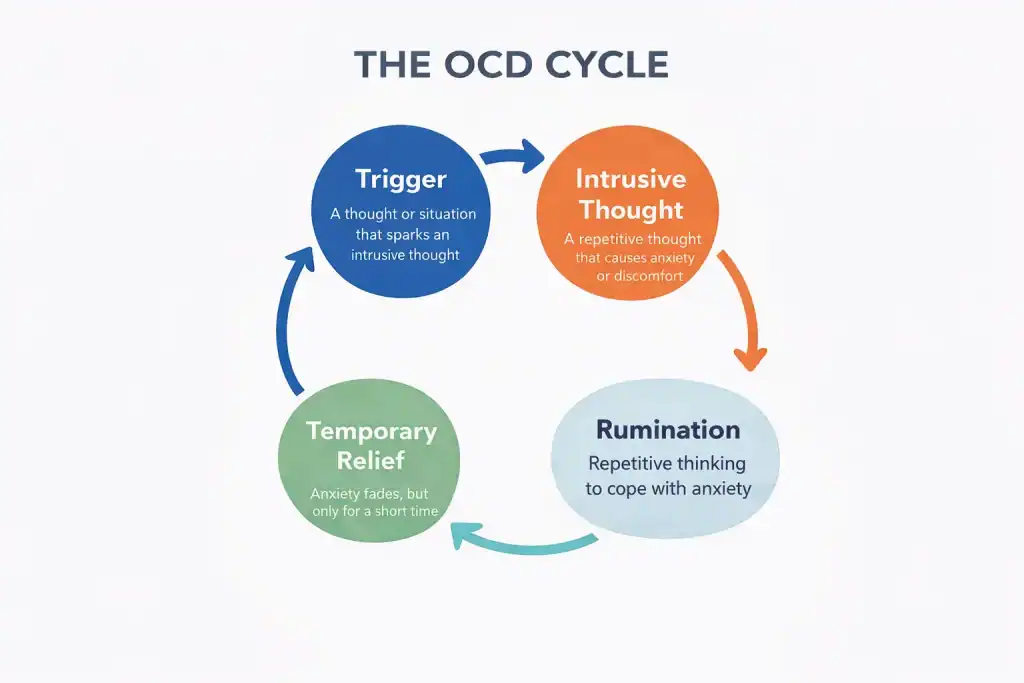
To escape the cycle, we need to let go of the notion that we need to “figure it out.” Instead, we first need to understand that ruminating doesn’t solve the problem. The next step is to become aware of the fact that we are ruminating. Only once we realize we are ruminating are we able to change this behavior.
ERP (Exposure and Response Prevention)
ERP is one of the most effective treatments for OCD and is a specific form of Cognitive Behavioral Therapy. It directly targets the cycle that keeps OCD going, which includes both obsessions and compulsions like rumination.
The key idea is response prevention, not thought suppression. You are not trying to get rid of the thought or prove it wrong, but rather to stop responding to it with compulsive thinking.
You allow the intrusive thought or doubt to be there without engaging in rumination. This means resisting the urge to analyze, solve, or mentally review, even when it feels uncomfortable or irresponsible to do so.
At first, this can feel very counterintuitive. Your mind will tell you that you need to figure it out, that this time is different, or that ignoring it could have consequences.
Over time, your brain learns that the anxiety can rise and fall on its own. When you stop feeding the cycle, the urgency of the thoughts begins to decrease, even if the thoughts themselves still appear.
This builds tolerance for uncertainty, which is at the core of OCD recovery. Instead of needing answers, you learn that you can handle not knowing, and that is what ultimately breaks the grip of rumination.
ACT (Acceptance and Commitment Therapy)
ACT takes a slightly different approach but complements ERP well. It focuses less on reducing symptoms directly and more on changing your relationship with your thoughts.
Instead of trying to control your thoughts, ACT focuses on building psychological flexibility. This means being able to experience difficult thoughts and feelings without getting stuck in them or letting them dictate your actions.
In practice, this means learning to notice thoughts without getting pulled into them. A ruminative thought can show up, and instead of analyzing it, you acknowledge it and allow it to pass without engaging.
For example, instead of getting caught in a loop of doubt, you might gently redirect your attention to a meaningful activity, even while the uncertainty is still present. The thought does not need to be resolved for you to move forward.
Over time, this creates space between you and your thoughts. You begin to see that thoughts are not commands or problems that must be solved, but mental events that come and go.
The goal is not to feel certain. The goal is to live well alongside uncertainty, guided by your values rather than by the need to eliminate doubt.
Medication
In some cases, medication can help reduce the intensity of OCD symptoms, including rumination.
Selective serotonin reuptake inhibitors, often called SSRIs, are commonly prescribed. They can make it easier to disengage from compulsive thinking and participate in therapy.
Medication is not a standalone solution for most people, but it can be a helpful support when combined with approaches like ERP or ACT.
Final Thoughts
OCD rumination is one of the most misunderstood parts of the condition. Because it happens internally, it can feel like “just thinking,” when in reality it is a powerful compulsion.
If you take one thing from this, let it be this:
You do not need to solve your thoughts.
The more you try to think your way out of OCD, the more stuck you become. Recovery begins when you step out of the loop, not when you win the argument in your head.
Rumination OCD FAQ
Overcoming rumination OCD involves recognizing rumination as a compulsion and resisting it. Approaches like ERP and ACT help you tolerate uncertainty without engaging in repetitive thinking.
Apps like NOCD, GG OCD, and mindfulness apps can support recovery by guiding ERP exercises, building awareness, and helping you disengage from rumination and compulsive thinking.
You do not ignore compulsions by force. Instead, you notice the urge and choose not to engage with it, allowing anxiety to rise and fall without performing the compulsion.
The 3-3-3 rule is a grounding technique where you name three things you see, hear, and feel. It can help shift attention away from rumination temporarily.