Key Takeaways
- ADHD and OCD can look similar on the surface, but they are driven by very different mechanisms: impulsivity and attention dysregulation vs anxiety and compulsions.
- ADHD pulls attention outward toward distractions, while OCD pulls attention inward toward intrusive thoughts.
- Both conditions affect executive functioning, which is why they are often confused or misdiagnosed, especially in children.
- ADHD and OCD can co-occur, but true dual diagnosis appears less common in adults than in children.
- Effective treatment depends on accurate diagnosis, as approaches differ significantly and some ADHD treatments may worsen OCD symptoms.
Disclaimer: This article is for educational purposes, not medical advice.
OCD vs ADHD: Understanding the Key Differences
At first glance, Attention-Deficit/Hyperactivity Disorder (ADHD) and Obsessive-Compulsive Disorder (OCD) can look surprisingly similar. Both can affect attention, focus, and daily functioning. Both often begin in childhood. And both are linked to difficulties with executive functioning.
But beneath the surface, they are very different conditions.
One helpful way to understand ADHD vs OCD is through the idea of externalizing vs internalizing disorders. ADHD is an externalizing disorder. It affects how a person interacts outwardly with their environment, often leading to impulsivity and risk-taking.
OCD, on the other hand, is an internalizing disorder. It involves turning inward, with intrusive thoughts and compulsive behaviors aimed at reducing anxiety.
Another way to contextualize this is to think of these disorders as part of the same continuum, the compulsive-impulsive continuum. OCD sits on the compulsive end, while ADHD sits on the impulsive end.
This difference shows up clearly in behavior. People with ADHD tend to be more impulsive and novelty-seeking. People with OCD tend to be more cautious, introspective, and risk-averse.
ADHD and OCD involve the same brain circuit, the frontostriatal system, but in opposite ways. ADHD is associated with underactivity, while OCD is linked to overactivity.
What Is ADHD?
ADHD is a neurodevelopmental condition characterized by persistent patterns of inattention, hyperactivity, and impulsivity. It is fundamentally about difficulty regulating attention, especially when tasks are not engaging.
ADHD is one of the most common psychiatric conditions in children. A large global study from 2007 estimated that ADHD affects about 5.2% of children and adolescents worldwide.
ADHD Symptoms and Behavior
ADHD is generally categorized into three presentations: predominantly inattentive, predominantly hyperactive-impulsive, and combined. These presentations describe which symptoms are most prominent, although they can change over time as a person develops.
Behaviors associated with predominantly inattentive ADHD include:
- Difficulty focusing or staying on task.
- Easily distracted by external stimuli.
- Forgetfulness and disorganization.
- Trouble following through on tasks.
Behaviors associated with predominantly hyperactive-impulsive ADHD include:
- Restlessness and difficulty sitting still.
- Talking excessively or interrupting others.
- Acting without thinking.
- Seeking stimulation or novelty.
What Is OCD?
OCD is a mental health condition characterized by a cycle of obsessions and compulsions. People with OCD often experience intrusive thoughts that cause anxiety and disrupt their lives. To cope with this anxiety, they often engage in compulsions.
OCD Obsessions and Compulsions
Obsessions are intrusive, unwanted thoughts, images, or urges that create anxiety or distress. In OCD, obsessions tend to be ego-dystonic, meaning that they are in conflict with the values of the person. For example, a person who cares deeply about their romantic relationship may experience intrusive thoughts about their partner not being “the one,” commonly known as relationship OCD.
Other common examples of OCD obsessions include:
- Fear of harming others.
- Fear that you may have done something terrible in the past without evidence.
- A sense that something is not “just right.”
- Fear of contamination.
Compulsions are behaviors or mental acts performed to reduce that anxiety. However, compulsions don’t work. While they may provide temporary relief, the anxiety or obsession always comes back stronger.
Examples of common compulsions include:
- Checking.
- Cleaning.
- Reassurance seeking.
- Repeating actions.
ADHD vs OCD: Key Differences
When comparing ADHD vs OCD, the differences become clearer:
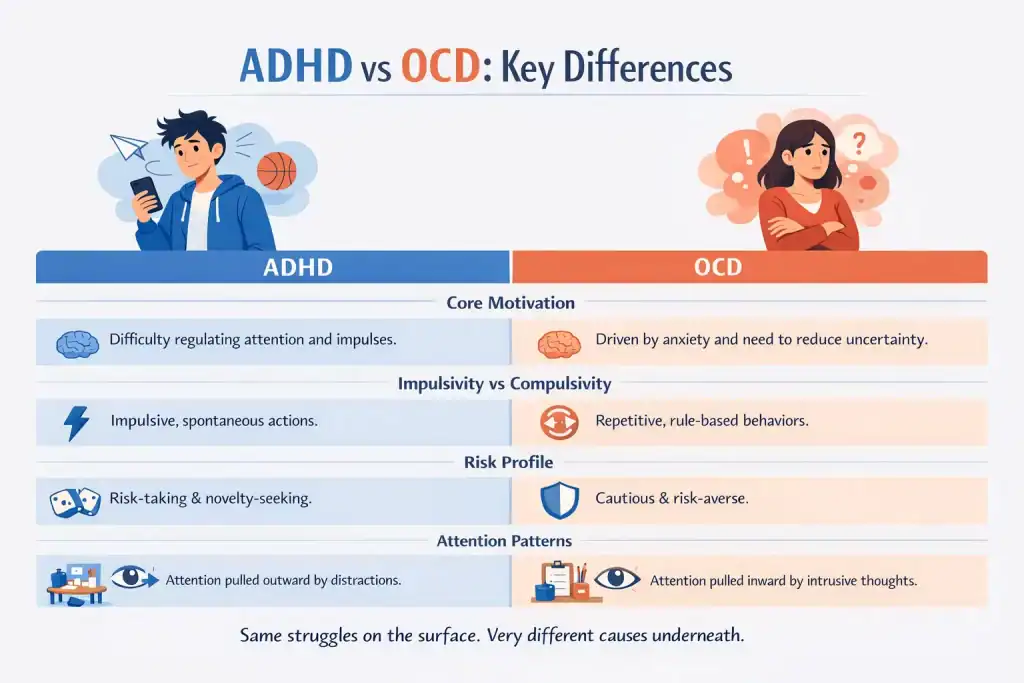
- Core motivation: ADHD is driven by difficulty regulating attention and impulses. OCD is driven by anxiety and the need to reduce uncertainty.
- Impulsivity vs compulsivity: ADHD involves impulsive behavior, while OCD involves repetitive, rule-based behavior.
- Risk profile: ADHD is associated with risk-taking. OCD, on the other hand, is associated with risk avoidance.
- Attention problems: ADHD attention is pulled outward by distractions. People with OCD, meanwhile, find their attention is pulled inward by intrusive thoughts.
- Behavior patterns: ADHD tends to be associated with disorganization, while OCD is often characterized by rigidity and excessive structure.
OCD and ADHD Overlap: Why They Can Look Similar
Even though the brain activity patterns differ in both conditions, both OCD and ADHD are associated with deficits in executive functioning, including planning, working memory, and response inhibition.
Due to these deficits in executive functioning, people with OCD or ADHD, or both, may struggle with focus, task completion, and organization.
There is also the idea of executive overload. In OCD, intrusive thoughts can overwhelm the brain’s capacity, making it difficult to focus on external tasks. This can make OCD look like ADHD, especially in children. Because of this overlap, ADHD and OCD are often misdiagnosed.
Can You Have ADHD and OCD Together?
While the common answer is “yes,” the picture is complex. According to the International OCD Foundation, results are inconsistent, with research showing a wide range of co-occurrence rates, from 0% to 59%.
For example, a 2006 study examined 94 children and adolescents diagnosed with OCD and found that over 25% of children and 17% of adolescents also had ADHD. Another study from 2010 reported a co-occurrence rate of 11.8%.
The International OCD Foundation says that 21% of children with OCD also have ADHD. For adults, the figure drops to 8.5%.
Meanwhile, a study from 2014 that assessed the neurobiological link between OCD and ADHD found that “ADHD was the most common comorbidity in early-onset OCD, in which tic and Tourette syndrome were exclusion criteria.”
However, the International OCD Foundation suspects that “full-blown dual diagnosis of ADHD and OCD in adults is in fact rather rare,” adding that ADHD-like symptoms in children with OCD may actually stem from OCD itself. As the brain develops, these symptoms may change or disappear.
Are OCD and ADHD Often Misdiagnosed?
Yes, OCD and ADHD are often misdiagnosed, largely because they can look similar on the surface. In both conditions, a person may appear distracted, unfocused, or disengaged. However, the underlying reasons for this distraction are very different.
In ADHD, attention is typically pulled outward by external stimuli. The person may struggle to stay focused because their mind is constantly shifting from one thing to another. In OCD, attention is pulled inward. The person may appear distracted because they are preoccupied with intrusive thoughts, doubts, or mental rituals.
Because both conditions involve difficulties with attention and executive functioning, clinicians may mistake one for the other. In some cases, OCD is misdiagnosed as ADHD. In others, one condition is identified while the other is overlooked entirely.
This is especially common in children, where diagnosis often relies on observations from parents and teachers. A child with OCD may seem inattentive in class, but the issue is not a lack of focus in the traditional sense. Instead, their attention is consumed by internal thoughts, such as worries, fears, or the need to mentally review something.
This is why understanding the difference between ADHD and OCD is so important. Without a clear distinction, the underlying problem can be misunderstood, leading to ineffective or even counterproductive treatment.
How OCD and ADHD Are Diagnosed
The diagnostic process for both OCD and ADHD typically involves a structured clinical assessment rather than a single test. Clinicians use standardized criteria, such as those outlined in diagnostic manuals, along with symptom checklists, interviews, and reports from the individual and, in the case of children, from parents or teachers.
The goal is to understand not just what behaviors are present, but why they are happening and how they impact daily functioning across different settings.
The International OCD Foundation recommends that clinicians pay close attention to two key factors when distinguishing between OCD and ADHD. The first is the presence of impulsivity and risk-taking. These traits are strongly associated with ADHD.
The second factor is the ability to perform detailed, repetitive behaviors that follow strict and often complex rules. This is a hallmark of OCD. People with ADHD, on the other hand, tend to struggle with sustained attention and consistency, making it difficult to follow through on complex, rule-based routines.
Ultimately, accurate diagnosis depends on understanding the underlying motivation behind the behavior. What may look similar on the surface can have very different causes, which is why a careful and thorough assessment is essential.
Causes of OCD and ADHD
Both ADHD and OCD arise from a combination of genetic, neurological, and environmental factors.
They involve the same brain circuit, the frontostriatal system, but in different ways. In ADHD, this circuit tends to be underactive, while in OCD it is overactive, leading to very different patterns of behavior.
The two conditions also involve different neurotransmitters. ADHD is primarily linked to dopamine, which affects motivation and attention, whereas OCD is more closely associated with serotonin, which plays a role in mood and anxiety regulation.
Treatment of ADHD and OCD
Treatment differs depending on the condition, although there can be some overlap in approaches.
For OCD, the most effective treatment is Exposure and Response Prevention (ERP), a form of Cognitive Behavioral Therapy (CBT) that helps individuals gradually face their fears without engaging in compulsions.
CBT more broadly can help challenge unhelpful thinking patterns, while Acceptance and Commitment Therapy (ACT) focuses on building psychological flexibility and changing the relationship to intrusive thoughts. In some cases, medication such as SSRIs may also be prescribed to help reduce the intensity of symptoms.
For ADHD, treatment typically focuses on improving attention, organization, and impulse control. This may include behavioral strategies, skills training for time management and focus, and medication, either stimulant or non-stimulant, depending on the individual’s needs.
When ADHD and OCD occur together, treatment becomes more complex and needs to be carefully balanced. For example, stimulant medication used for ADHD may sometimes worsen OCD symptoms in certain individuals. For this reason, it is important that treatment is guided by a clinician who can monitor symptoms closely and adjust the approach accordingly.
ADHD vs OCD FAQ
Neither ADHD nor OCD is inherently “worse.” Both can significantly impact daily life in different ways. OCD often involves intense anxiety and distress, while ADHD affects attention and impulse control. Severity depends on the individual and how symptoms interfere with functioning.
Both are diagnosed through clinical assessments, not lab tests. ADHD evaluation focuses on attention, impulsivity, and behavior across settings. OCD assessment focuses on intrusive thoughts and compulsions, including their frequency, distress, and impact on daily life.
ADHD is commonly treated with stimulant or non-stimulant medications that target attention and impulse control. OCD is typically treated with SSRIs, which help regulate anxiety. Medication choice depends on symptoms and should be guided by a qualified clinician.
Look for licensed psychologists or psychiatrists with experience in both ADHD and OCD. Specialists in anxiety disorders or neurodevelopmental conditions are ideal. Reputable directories, such as professional associations or mental health organizations, can help you find qualified providers.

Leave a Reply